In pioneering research, Canadian scientists have successfully used gene therapy to repair damaged lungs from deceased donors, making them potentially suitable for life-saving transplantation.
More than 80 per cent of donor lungs are discarded because they are not healthy enough to be transplanted in a recipient, says principal researcher Dr. Shaf Keshavjee, senior scientist at the McEwen Centre for Regenerative Medicine in Toronto.
Keshavjee said the gene therapy, developed by a team at the University Health Network centre after more than 10 years of research, could potentially expand the number of viable donor lungs as well as improve the outcome for patients receiving a transplant.
“I think the exciting thing here is the proof of concept, that you can diagnose what’s wrong with an organ and genetically modify the organ to work better after transplantation,” he said. “So it really opens the door to personalized medicine for organs that we transplant.”
The technique involves removing the lungs from a deceased donor and placing them in a special perfusion unit that pumps oxygen, nutrients and other substances into the organs, as if they were breathing inside a body.
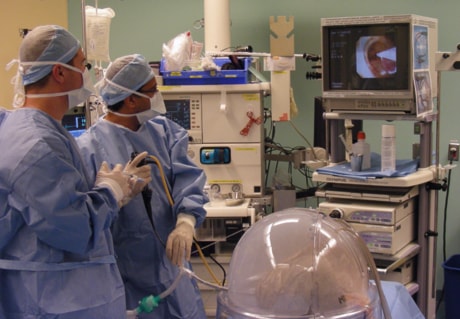
The gene therapy is then introduced through a bronchoscope — a long tube-like apparatus fitted with a miniature camera, which allows doctors to watch on a screen as the scope is fed through airways and then into deeper areas of the lungs.
Using a tiny catheter attached to the scope, they squirt in the treatment — a liquid containing multiple copies of a cold virus that’s had its own genetic machinery replaced by a human gene called interleukin-10.
“And then with the breathing movement of the ventilator, it disperses it into the lung,” Keshavjee said.
When these disabled cold viruses infiltrate the lung tissue, the IL-10 gene they carry begins producing a protein that helps the organs heal their injured cells.
“You make each cell that’s transduced (genetically altered) into a little IL-10 factory to locally produce IL-10 in the lung,” said Keshavjee, explaining that the gene therapy keeps working for about a month.
In a report published Wednesday as the cover story in the journal Science Translational Medicine, Keshavjee’s team compared sets of donor lungs, some maintained in the perfusion system without intervention and some treated with the IL-10 gene therapy.
They found that the first set of lungs did not deteriorate and remained stable in the dome-like ventilating device.
But those lungs also treated with gene therapy had significantly improved blood flow and a better ability to take in fresh oxygen and expel carbon dioxide.
The researchers say that transplanting lungs which function better from the start would lead to more predictable, safer outcomes for recipients, with shorter periods of mechanical ventilation and intensive care stays.
“Everything we can do to prevent lung injury, especially in the first 72 critical hours after surgery, would have a significant impact on survival and quality of life after transplantation,” said co-author Dr. Marcelo Cypel, a transplant surgical fellow at Toronto General Hospital.
Patients with severe early lung injury are at greater risk of dying after surgery, and have higher rates of organ rejection later on, Cypel said.
Keshavjee said IL-10 not only helps restore healthy lung tissue prior to transplant, but also reduces inflammation and tamps down signals that would set off an attack by immune system cells that cause organ rejection.
While a long way off, it’s possible that different kinds of gene therapy could some day do away with the need for patients to take lifelong anti-rejection drugs, which suppress the immune system and leave a transplant recipient vulnerable to infections and some kinds of cancer.
It might be possible, he said, to use such therapies to protect an organ from rejection, while not interfering with the immune response in the rest of the body. The research team, which has successfully transplanted treated lungs in rodents and pigs, hopes to begin offering restored human lungs to patients within a year or two as part of a clinical trial.
They estimate that the number of donor organs available for lung transplants could easily be doubled with the gene-therapy — providing a much-needed increase in supply.
In Canada, the number of people waiting for a lung transplant has doubled in the past 10 years. In 2006, 252 Canadians were on the waiting list, compared to 119 in 1997.
Almost 300 people needing a new lung died during that nine-year period.
But Keshavjee said lungs may not be the only organ that can be rescued with gene therapy. Down the road, the treatment potentially could refurbish damaged hearts, livers and kidneys.
“This work opens the door for a variety of therapies that could potentially be applied to repair various injuries in other donor organs to improve the safety and outcome of transplants.”
In an accompanying commentary, Dr. David Wilkes of the Indiana University School of Medicine, called the research “an important translational advance in the field of lung transplantation.”