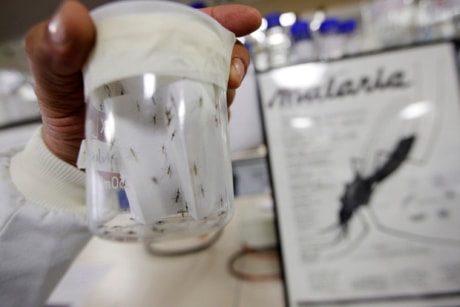
LONDON — In a cramped London laboratory filled with test tubes, bacteria and mosquitoes, scientists are trying to engineer a new weapon in the battle against malaria: a mutant fungus.
For years, Angray Kang at Westminster University and colleagues have been testing whether they could genetically tweak a fungus to kill the malaria parasite carried by mosquitoes.
Now they’ve found that in lab experiments, mosquitoes exposed to the fungus show a sharp drop in levels of the parasite. If it works that way in the wild, that should make it harder for the disease to infect people.
Kang said the mutant fungus could be sprayed onto walls and bednets like insecticides and could be made for a comparable cost.
He said the same process of genetic modification could also be used to target other insect-spread diseases like dengue and West Nile virus. The research was done together with scientists at the Johns Hopkins School of Public Health and was funded by the U.S. National Institutes of Health. Early results were published recently in the journal Science.
“This is very exciting research,” said Andrew Read, director of the Center for Infectious Disease Dynamics at Pennsylvania State University. He has worked on similar projects but was not involved with the fungus research. “It tells us that if you can’t find something in nature to do what you want, you can just make it.”
Read said using the souped-up fungus might be less environmentally invasive than other genetic approaches. Some critics have warned that competing biological approaches, like scientists creating mutant mosquitoes, could wreak havoc to ecosystems if billions of the insects are released into the wild.
With the fungus, “you just spray it on the wall and it does its job,” Read said. “You don’t have to worry about generation after generation of the stuff.”
He also said the fungus technology could be a new way of dealing with insecticide-resistant mosquitoes, an increasing problem that has meant the return of effective but controversial sprays like DDT. “With the (mutant) fungi, you wouldn’t have chemical residues hanging around,” he said. “It would just be a fungus very similar to what is already found in nature.”
In laboratory tests, Kang and colleagues found mosquitoes exposed to the mutated fungus had malaria parasite levels about 85 per cent lower than normal. When they added a scorpion toxin to the mix, levels dropped by 97 per cent. No tests have shown whether using the fungus would curb human malaria cases, but experts think fewer malaria parasites should translate into fewer cases.
“If the strategy works and there are fewer parasites, this could change how malaria is spread and reduce transmission to humans,” said George Christophides, an infection expert at Imperial College London who was not associated with the research.
Kang’s experiment involved inserting a human antibody against malaria into a fungus commonly found in soil and plants worldwide. Spores made by the fungus burrow into the mosquito, invading its circulatory system. When the malaria-causing parasite multiplies inside the insect, the antibody keeps the parasites from reaching the mosquito’s salivary glands. That theoretically stops the disease’s spread.
“The mosquito can be infected by malaria, but it can’t pass it onto humans,” Kang said. The mutated fungus then eats away at the mosquito from the inside, killing the insect after a couple of weeks. That’s long enough for the mosquito to reproduce, which should lessen its incentive to evolve resistance to it.
The same fungus — minus the genetic modifications — is already produced in industrial quantities to squash locust outbreaks in Australia. The fungus is naturally lethal to locusts, so no genetic modification is needed.
If Kang and colleagues can get enough funding, they hope to test the mutant fungus in malaria-endemic countries like Burkina Faso, Kenya or Tanzania.
Other experts doubted whether the laboratory experiment could be replicated in the wild. “It’s a neat scientific idea, but there are questions about (the mutated fungus’s) stability and formulation,” said Janet Hemingway, director of the Liverpool School of Tropical Medicine. She said the mutant fungus would have to survive being shipped to Africa and then be viable for another three to six months in stifling heat once it’s sprayed onto walls or bednets.
One group that campaigns against genetically modified organisms warned the mutant fungus could skew behaviours of other wildlife.
“The release of any genetically modified organism into the environment runs the risk that it may have wider impacts than just its target,” said Pete Riley, campaign director of GM Freeze, a U.K.-based advocacy group. He said the modified fungus could have unintended consequences which might be impossible to reverse. “Nature has a pretty cunning way of getting around everything we throw at it,” he said.
Kang acknowledged that simply having a new mutant fungus would not stop malaria. “We still need better drugs and other interventions,” he said. “But malaria kills about a million people every year so we have to try whatever may work.”