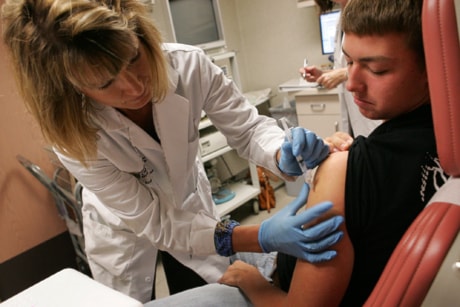
TORONTO — With fears that Canada could be hit by a massive wave of H1N1 influenza cases this fall, nurses across the country are preparing to take their places on the front lines of the pandemic — and bracing for the worst.
For months, provincial and territorial nurses groups have been engaged in pandemic planning with hospitals and government, while readying their members for a possible onslaught of cases that could swamp the system.
One of the greatest concerns is that there simply will not be enough nurses to handle a sustained influx of patients, especially those admitted with life-threatening complications.
While most cases of H1N1 so far have caused only mild symptoms, a proportion of those infected have become seriously ill, ending up in intensive care units on ventilators, often for weeks.
“If I was to look at the biggest threat, I think it’s the lack of us having the capacity for the surge or the need for RNs on the front lines,” says Linda Haslam-Stroud, president of the Ontario Nurses’ Association.
There is already a shortage of nurses in the health-care system, she says. If swine flu does hit with a vengeance, it’s likely some health-care workers will be among those who contract the infection.
“So we’re in a situation where these nurses are not going to have enough colleagues to care for patients.”
Sandi Mowat, president of the Manitoba Nurses Union, says Winnipeg hospitals have already experienced a sudden flood of swine flu patients needing specialized treatment.
In June, the virus swept through several northeastern aboriginal communities, leaving a trail of infectious destruction that saw dozens of patients airlifted to three Winnipeg hospitals.
“We had like a six-week surge in this province of very sick, high-acuity patients requiring ventilator care,” she recalls. “Our ICU bed counts were at a maximum. We were actually over what our normal city ICU bed counts would be.”
“And the end result was we didn’t have nursing staff for those beds,” says Mowat, adding that hospitals had to transfer RNs with previous ICU experience from other departments to help ease the shortfall.
Beyond adequate staffing levels, nurses are adamant that their working environments be as safe as possible — with appropriate protective gear like properly fitted N95 masks — and that they be kept informed by daily communication with hospital administrators.
They don’t want a repeat of what happened during the 2003 SARS outbreak that killed 44 people in the Toronto area.
“SARS is still in the forefront of the nurses’ minds across Ontario, obviously,” says Haslam-Stroud. “Although it might seem like a long time ago to the public, it isn’t a long time ago to the nurses who were in the trenches. We had two of our nurses die of SARS.”
“I think the difference now is that nurses are very clear in saying they want to be on the front lines — that’s what they’re trained to do — but they are not willing to put themselves at risk like they did during SARS.”
Among them is Kim Campbell, who contracted SARS during a second wave of the epidemic that struck Toronto’s North York General Hospital after the province prematurely declared the threat had been contained.
Like other nurses stricken by severe acute respiratory syndrome, Campbell is still dealing with the physical and cognitive scars left by the disease, which put her in hospital for a week and required lengthy rehabilitation.
While back to full-time hours now, the mother of three continues to experience fatigue, has painful joint problems and becomes short of breath with any exertion. Her memory has also been impaired.
The emergence of the new H1N1 flu strain in April rekindled the anger and fear she felt over SARS and thought she had put behind her.
“They kept talking about it more and talking about the pandemic and what level it was. I got really scared.”
“I went to my boss and I said, ‘I just want to tell you if it gets worse, if it gets to the point where we’re masked and gowned, I can’t do it.’ . . . I just said to her I can’t work.”