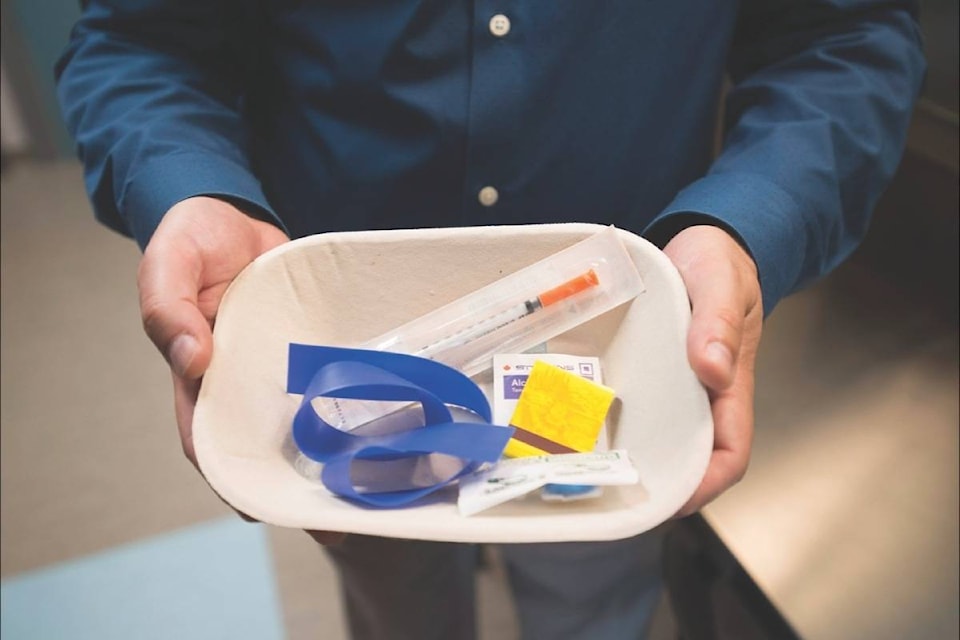
SURREY, B.C. — Drug users will start injecting their own heroin or other illicit substances at a new supervised injection site opening this week in Surrey, B.C., in efforts to curb a crisis in overdose deaths.
SafePoint will be British Columbia’s first site outside of Vancouver that allows people to shoot up drugs under medical supervision while they are linked up with other health and social services.
A similar service will be incorporated later this month into an existing clinic in Surrey, which has had the second-highest number of overdose fatalities in the province after Vancouver.
The BC Coroners Service has reported that of the 931 overdose deaths in the province last year, 108 occurred in Surrey. There were 51 overdose fatalities in the first four months of this year in the city.
SafePoint is set to open on Thursday and comes 14 years after the groundbreaking start of Insite in Vancouver in the midst of an HIV epidemic.
Just like at Insite, intravenous drug users will be given clean needles at individual booths where they can inject drugs while being monitored by staff ready to administer the overdose-reversing drug naloxone if necessary.
Anyone who uses illicit substances in a supervised injection site approved by Health Canada is exempt from the country’s drug laws.
Dr. Victoria Lee, Fraser Health’s chief medical health officer, called the department’s approval of SafePoint bittersweet, saying the health authority submitted an application requesting that users also be allowed to snort drugs or take them orally.
“We know that people are dying not only from injecting drugs but orally consuming and inter-nasally consuming as well, and we wanted to provide them with supervised consumption services as well,” Lee said Tuesday outside the new facility.
She said that’s essential because of a public health emergency declared by the province in April 2016 over an unprecedented number of overdose deaths that continues to rise.
Some drug users living in about 70 tents across the street from SafePoint said they would not inject at the clinic because there is a community RCMP policing station next door.
Lee said several surveys of community organizations and substance users suggested people would inject at the facility despite the presence of police nearby.
“We will monitor what the uptake looks like. If we see that if the uptake is not what we expected we will look with our partners, community organizations as well as RCMP and local municipal stakeholders to improve access,” she said.
Fraser Health said in a statement that there are more than 500 visits each week to a nearby overdose prevention site, though some people in the tent city said they would continue going there instead of SafePoint.
One drug user, who did not wish to be named, said there’s a more urgent need for housing in Surrey, which, unlike Vancouver, does not have single-room occupancy hotels for people who live on the street or go to shelters.
Lee acknowledged the lack of housing as a problem.
“There are new builds underway,” she said, adding the Lookout Emergency Aid Society, which has been contracted to operate SafePoint, also manages shelters in the city.
Former drug user Karen Scott told a news conference at SafePoint that she was addicted to crystal methamphetamine and unwittingly took some laced with fentanyl before entering a treatment program involving the drug suboxone.
Scott urged drug users to take advantage of SafePoint, noting the same treatment, along with methadone, will be offered adjacent to the new clinic.
Besides Insite, a smaller supervised injection site run by the Dr. Peter AIDS Foundation also exists in downtown Vancouver.
Health Canada said Tuesday that it has approved 12 applications for supervised injection sites elsewhere: four in Montreal, including one mobile unit, and three in Toronto, although they have not yet opened.
The department said 12 applications are under consideration, including three from other cities in B.C., four from Edmonton, one from Calgary and three from Ottawa.
— Follow @CamilleBains1 on Twitter.
Camille Bains, The Canadian Press