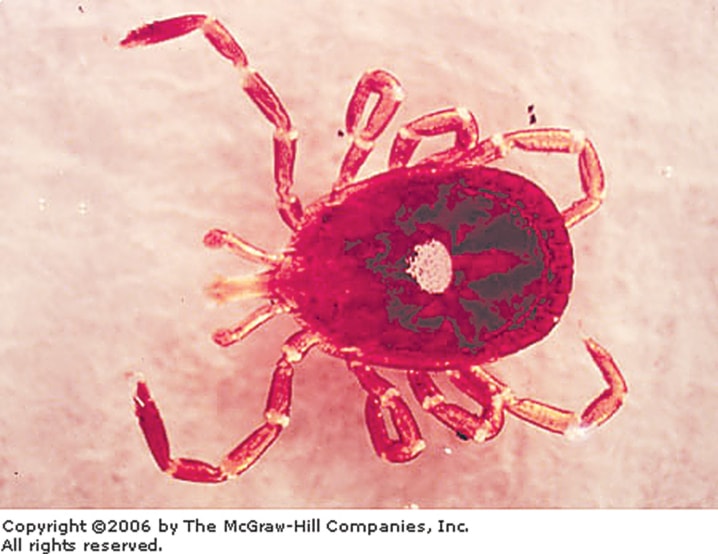
It’s the middle of the dog days, which, oddly enough, can bring a respite from an onslaught of ticks in some parts of North America.
Generally, U.S. experts say the risk of tick encounters is low from the Ohio Valley and west of the Mississippi, and medium from the Deep South and eastward across the rest of the country
But just because hot, sultry days might make arachnids a bit less active now than during the spring and early summer, they’re no less likely to hitch on when given a chance. And bloodsuckers in the smaller, nymph stage of their life cycle are just as capable of sharing illness with humans as they will be as adults come fall.
Depending on your location, the threats range from Lyme disease, anaplasmosis and babesiosis to Rocky Mountain spotted fever and several similar fevers, tularemia, and even the onset of a nasty allergy to red meat.
A July report from researchers at Virginia Commonwealth University documents three patients who developed a severe, life-threatening reaction to beef in response to a bite from a tick — one named the Lone Star tick, to add insult to injury. This species is the one most likely to be encountered from Maryland to Florida during this part of the season.
Drs. Susan Wolver and Diane Sun and colleagues from the University of Virginia report that the delayed allergic reaction showed up roughly three to six hours after each patient ate red meat. They typically suffered from hives, an itchy rash and/or anaphylaxis — a reaction marked by closed airways and throat, abdominal cramps, nausea and a drop in blood pressure among other symptoms. The reactions can be fatal if left untreated.
The researchers think the reaction is caused by antibodies to a carbohydrate, called alpha-gal, which is produced in the blood in response to the bite of the Lone Star. The same carb is present in most meat — beef, pork, lamb and venison.
So when someone who has been bitten by a Lone Star tick eats the meat, the immune system reacts to the carb by releasing a surge of histamine that produces the allergic reaction.
The study, published online in the Journal of General Internal Medicine, suggests that doctors need to be aware of the new syndrome when they encounter patients suffering from allergic reactions, and may have to counsel them to avoid meat from mammals.
The Lone Star tick can also produce an after-bite rash and reaction that’s often confused with Lyme disease. It’s been named Southern Tick-Associated Rash Illness, although the Lone Star’s range has expanded north into New England and westward into the Plains. The rash can be accompanied by fatigue, headache, fever and muscle pains, but the exact cause of the illness is not known.
Lyme disease itself is transmitted by deer ticks, or blacklegged ticks, which have been spreading into new areas throughout the century, particularly in the upper Midwest. Although the ticks rely on deer to reproduce, they pick up the bacteria that cause Lyme from mice and other small mammals.
For instance, a study by researchers at the University of Illinois published last year noted that deer ticks are established in at least 26 counties, up from eight in 1998. Tick counting and testing showed that infected ticks were more likely to be found on prairie and young forest land than in mature forest, with more ticks per animal on prairie voles than the typical host, white footed-mice.
Along with Lyme, deer ticks seem to be spreading babesiosis across more of their range.
The disease, caused by a parasite that attacks blood cells, results in flu-like symptoms such as fever, chills, fatigue and head and muscle aches. First documented in Massachusetts in 1969, more than 1,200 cases were reported to the federal Centers for Disease Control and Prevention in 15 states last year.
Experts say many more people are probably infected with the parasite and have no symptoms. The disease can be treated with antimicrobial drugs, but it can be fatal to anyone with a weakened immune system, including the elderly, people fighting cancer, HIV or without a spleen.
The infection may be harder to diagnose because there’s no rash and the tick and its bite are miniscule. Lab inspection of a blood sample under a microscope is currently the only way to confirm infection.
In the West, the main summertime danger from ticks is tick-borne relapsing fever, a bacterial illness spread from mice and other rodents through several species of long-lived “soft” ticks. The threat is greatest for people who sleep in rustic cabins or summer homes.
For more information of tick-borne illness, go to: www.cdc.gov/ticks. Or www.tickencounter.org
Lee Bowman is a health a science writer for Scripps Howard News Service. Contact Bowman at BowmanL@shns.com